This article examines the extent to which research of alcohol abuse, illicit drug use, and prescription drug abuse among older adults seem in the main gerontological and substance abuse journals.
The authors reviewed articles printed in the 10 social science gerontological journals and the 10 social science substance abuse journals with the best 5-year influence components in PubMed from 2000 to 2010.
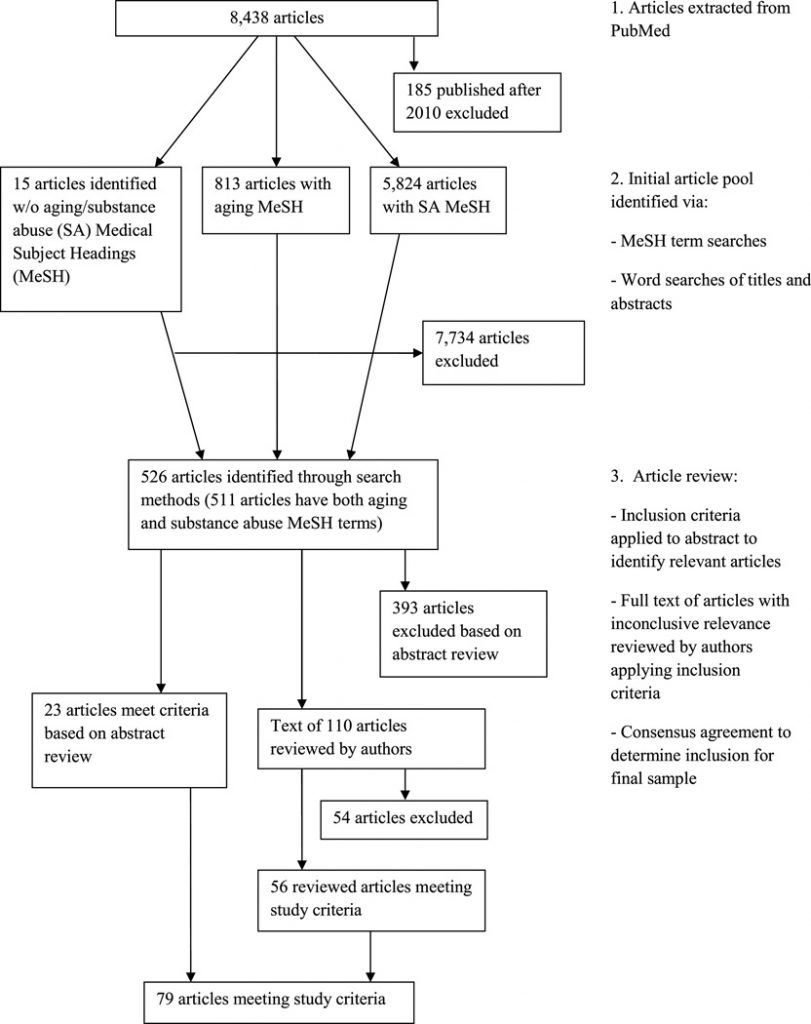
Articles have been chosen that introduced authentic analysis on alcohol, substance, or prescription abuse with older adults aged 50 and older; and have been recognized by way of getting old and substance abuse-related Medical Subject Headings and phrase searches of titles and abstracts (N = 634). Full textual content of every article was reviewed by the authors, and consensus decided inclusion in the ultimate pattern.
Of the 19,953 articles printed respectively in the highest 10 gerontological and substance abuse journals, 181 articles met the inclusion standards of reporting findings associated to substance use disorders among older adults. Specifically, 0.9% (102 of 11,700) of articles from the highest 10 gerontology journals and 1.0% (79 of 8,253) of articles from the highest 10 substance abuse journals met the factors.
Most printed articles addressed alcohol misuse/abuse or polysubstance abuse with few articles addressing illicit drug use or the misuse of prescription medicines. Less than 1% of articles printed in the 10 gerontology journals and the 10 substance abuse journals with the best 5-year influence scores addressed substance abuse in older adults.
Practitioners treating well being and/or psychological well being issues are at a drawback in precisely figuring out and treating these situations in older grownup populations with no correct understanding of the position of comorbid substance use disorders.
Socio-demographic and scientific profile of persistent ache with neuropathic traits in sub-Saharan African aged.
Data on traits of neuropathic ache (NP) in sub-Saharan Africa are scarce, particularly in the aged. We carried out this research to understand the socio-demographic and scientific profile of persistent ache (CP) with neuropathic traits in sub-Saharan African aged with musculoskeletal ache.
From January to December 2011, we carried out a cross-sectional research in all Rheumatology outpatients over 60 years on the Center for Gerontology and Geriatrics, Dakar, Senegal. In this research, we included sufferers who skilled musculoskeletal ache for Three months or longer (CP) and with a DN4 rating ≥ 4 (NP). An entire scientific examination was carried out to make the prognosis of NP ‘particular’ or ‘possible’, and to determine the aetiologies of NP.
During the research interval, 698 outpatients have been examined. There have been 394 out of the 549 sufferers over 60 years who reported CP. Among them, 28 sufferers (7.1%) scored ≥Four on the DN4 questionnaire. Female sufferers, low instructional attainment, guide professions, non-workers and diabetes have been related to NP (p < 0.05). The signs described by sufferers with NP, usually intricate, have been lumboradiculalgia (n = 9), cervico-brachial neuralgia (n = 3), polyneuropathy (n = 12) and mononeuropathy (n = 6). The presumed aetiologies in sufferers with NP have been: persistent backbone ailments (n = 14), painful diabetic peripheral neuropathy (n = 8), Sjögren’s syndrome (n = 1), tarsal tunnel syndrome in rheumatoid arthritis (n = 1) and bone metastasis (n = 1).
No aetiology was recognized among three sufferers. Chronic backbone ailments related to radiculopathies and diabetic neuropathy are the principle causes of NP, nicely detected by DN4 questionnaire and scientific examination in Senegalese sub-Saharan African aged.
